People coming to Southside Physiotherapy Clinic frequently ask what is osteoporosis? 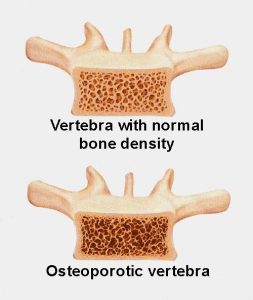 Osteoporosis is a condition where there is thinning of the bones, causing them to fracture (break) more easily.
Osteoporosis is a condition where there is thinning of the bones, causing them to fracture (break) more easily.
What happens to the bones?
Bone is a living tissue, which is made up of a hard outer shell and an inner honeycomb structure, consisting of tiny collagen fibres and minerals such as calcium and phosphate. These minerals determine the bone mass or density, and are what give bone its strength.
Bone is constantly being renewed by a process called bone remodelling or bone turnover, in order to maintain its strength. Old, worn-out bone is constantly being broken down by a type of bone cell called osteoclasts, and replaced with new, stronger bone by cells called osteoblasts.
During childhood and adolescence, bone is produced faster than it is broken down, leading to an overall gain in bone. The amount of bone in the skeleton reaches its maximum by the mid-20s this is called peak bone mass.
After the mid-30s, bone is broken down faster than it is replaced. A certain amount of decrease in bone density with age is therefore natural. However, in people with osteoporosis, the bone density becomes abnormally low meaning the bones are fragile and more likely to fracture.
What causes osteoporosis?
There are a number of reasons why osteoporosis or bone thinning can develop. A major reason is if the bones were not very strong to begin with (i.e., if peak bone mass was low). If this is the case then osteoporosis will be more likely to develop during the natural decline of bone mass with age.
There are a number of factors which determine peak bone mass, although not all of them are fully understood. They include:
- Calcium intake
- Genetic (hereditary) predisposition
- Physical exercise
- Sex hormones
Osteoporosis can often occur after the menopause in women. This is due to a decline of the female hormone oestrogen, which causes a marked decrease in bone density.
Other medical conditions can also sometimes lead to osteoporosis. These include conditions that affect the absorption of food, such as Crohn’s disease, coeliac disease and ulcerative colitis, and conditions that leave you immobile, such as arthritis. Use of corticosteroid tablets can also increase risk of osteoporosis.
How common is osteoporosis?
Osteoporosis affects one in three women and one in five men over the age of 50. The prevalence of the disease increases with age: two thirds of women aged 80 and over are affected.

How is Osteoporosis Diagnosed?
If you suspect you have osteoporosis or if you feel you may have a chance of developing it, for example if it runs in the family, visit a doctor.
Your doctor will take a detailed medical and family history, which will help to determine your risk of developing osteoporosis. Established osteoporosis may be visible on routine X-rays, but this is not always the case.
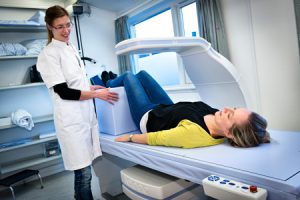
If osteoporosis or slight bone thinning is suspected, a type of bone scan called a bone densitometry scan (DXA scan) can be carried out to measure the density of the bones. It is a simple, painless procedure that uses very low doses of radiation to scan the lower spine and the hip. It is currently the most accurate and reliable means of assessing the strength of your bones and your risk of breaking a bone.
If you are found to have osteoporosis or osteopaenia, your doctor will make a number of recommendations, which may include medication and/or lifestyle changes.
The Irish Osteoporosis Society recommends that you are scanned every two years after your initial scan.
Why exercise?
The importance of exercise for maintaining strong, healthy bones cannot be underestimated. Bones need regular weight-bearing exercise. Exercise stimulates bone, creating bone turnover, growth and strength. It will also help to rebuild bone in those who have already developed osteoporosis, and it can also provide relief from osteoporosis pain. .While cycling and swimming are excellent activities for overall fitness they do not benefit bone strength as they are not weight-bearing. President of the Irish osteoporosis Society, Prof Moira O’Brien, recommends 30 minutes of daily weight-bearing exercise for all age groups, including senior citizens. Why is Physiotherapy beneficial? A study in the US and Japan, found that older, postmenopausal women, who used small weights to strengthen their back muscles over a period of two years, were less likely to get vertebral fractures. In fact the back strengthening exercises reduced the chance of getting a fracture by almost threefold. In the women aged 58 to 75 years, only one in 10 of those who exercised were found to have a vertebral fracture, while almost one-third of the women in the group that had not used the exercise regimen had suffered a fracture. Women who had not taken part in the back exercise programme were also about twice as likely to have a compression fracture in the spine. This can lead to a hump developing on a person’s upper back, a very painful condition which increases the risk of falling.
Participating in a Physiotherapy lead group class with weight bearing exercises tailored to your level will stimulate bone and improve your bone health.
